#amyloid-beta
#amyloid-beta
[ follow ]
fromNews Center
3 weeks agoCalcium Signaling Channels Regulate Neuroinflammation and Motivation - News Center
This could open up some interesting possibilities for therapeutic interventions for depression-like behaviors or maladaptive changes in motivational behaviors down the road where microglia are known to play a really important role.
Science
#dementia
Parenting
fromSilicon Canals
3 weeks agoThe cruelest thing about dementia isn't the forgetting - it's the afternoon your mother looks at you with perfect clarity, says something so sharp and specific it could only come from the woman she was before, and then it closes like a window, and you spend the drive home trying to decide if that moment was a gift or the worst kind of goodbye - Silicon Canals
Moments of clarity in dementia patients are emotionally devastating because they offer false hope before the person disappears again into confusion.
Medicine
fromNews Center
2 weeks agoSchizophrenia Study Finds New Biomarker, Drug Candidate to Treat Cognitive Symptoms - News Center
Northwestern researchers identified a novel schizophrenia biomarker in cerebrospinal fluid that could enable new treatments for cognitive symptoms through a synthetic protein therapeutic approach.
fromwww.scientificamerican.com
3 weeks agoThe gut microbiome may influence brain aging, mouse study suggests
Young, two-month-old lab mice housed with older, 18-month-old mice showed really impaired cognition. Researchers exposed young mice raised in a sterile, microbe-free environment to gut bacteria from old mice, causing the younger animals to perform worse on cognitive tests, as if they had prematurely aged, just like the cohoused mice.
Medicine
fromPsychology Today
1 month agoCould Glial Cells Be the Key to New Schizophrenia Treatments?
Anyone living with schizophrenia understands the true limitations of current treatment options. Antipsychotics remain the single leading treatment for the disorder, and they are riddled with undesirable side effects. Weight gain, tardive dyskinesia, and excessive drowsiness are a few. Much research is devoted to expanding the range of medication options, and few academics have pursued other avenues. However, there is a possibility that treatment for schizophrenia can be approached through cellular methods if long-term research validates early signs of hope.
Mental health
fromPsychology Today
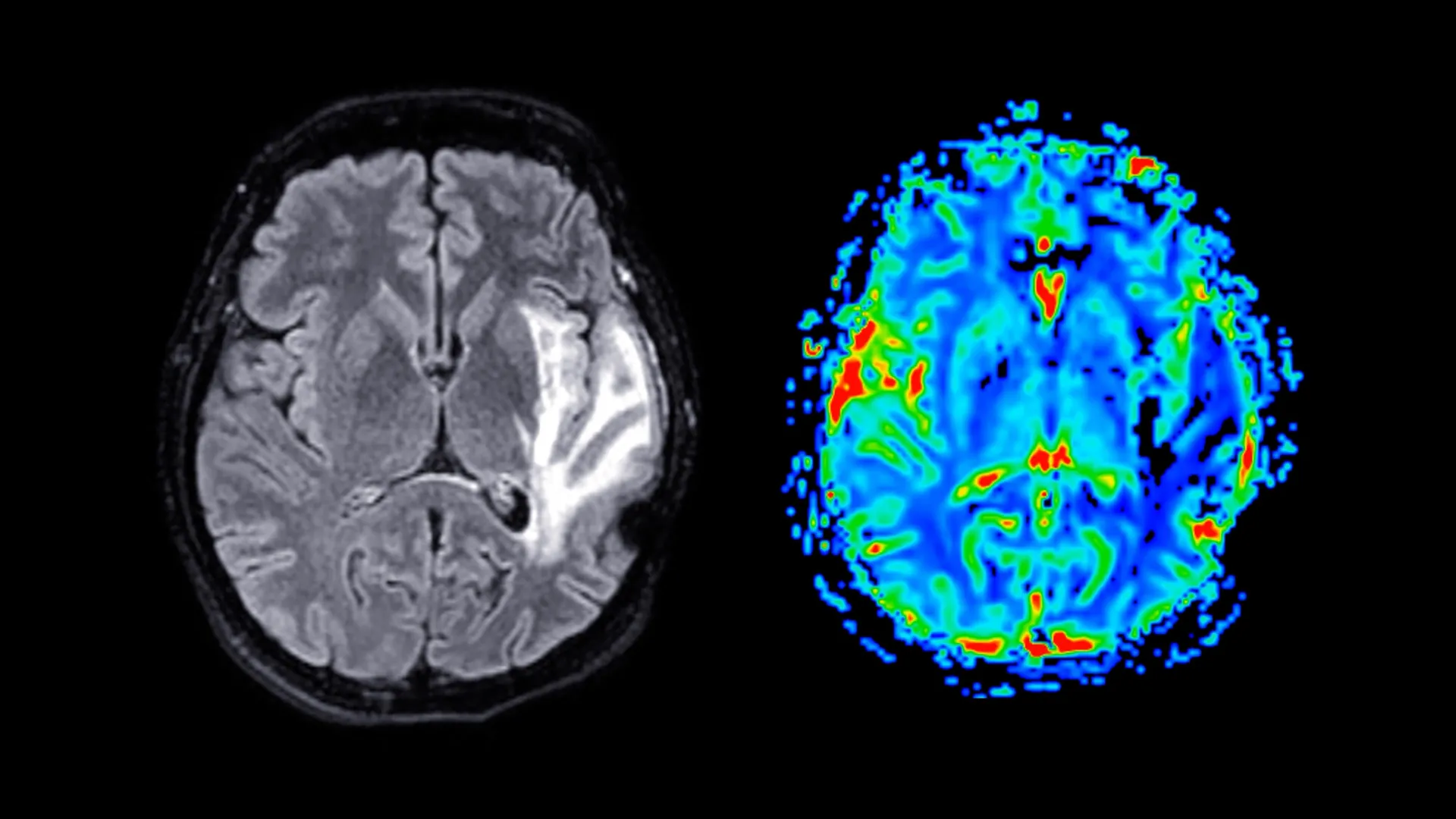
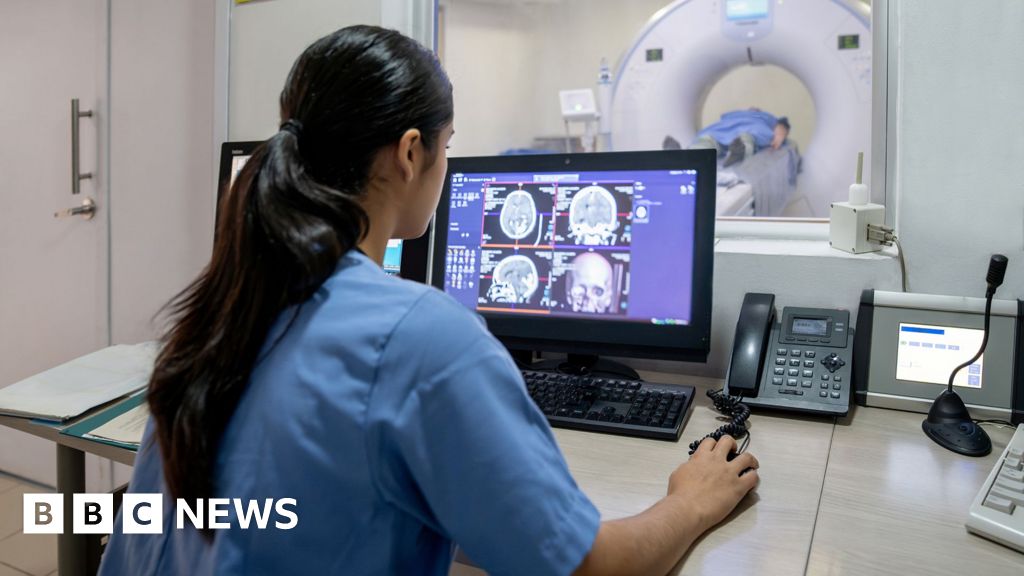
1 month agoAI Spots Brain Disorders in Seconds From Scans
According to University of Michigan neuroscientists, not only can their AI vision language model diagnose neurological disorders from MRI scans with high performance accuracy, but it also has foundation model capabilities, making it a flexible, general-purpose solution that can be tailored for a wide variety of medical imaging. "These results demonstrate that Prima has foundation model properties, and reported performance will continue to improve with additional health system training data and larger compute budgets," wrote the study's authors in the preprint.
Artificial intelligence
fromSilicon Canals
1 month agoNeurologists reveal the everyday habit that doubles your dementia risk - Silicon Canals
A groundbreaking study found that adults who sit for 10 or more hours daily face a significantly higher risk of dementia compared to those who sit less. The research, which tracked over 50,000 adults using wearable devices, revealed that the risk increases dramatically after crossing that 10-hour threshold.
Health
fromPsychology Today
2 months agoWhen Memory Worries Deserve Attention
Most people will forget a name, misplace their phone, or lose track of a conversation at some point. Usually, those moments pass without much thought. But for many adults, especially as they age, small lapses can trigger a much deeper fear: Is this the beginning of cognitive decline? As a neurologist, I hear this concern often. And as a researcher, I have learned something important: Worry about cognition and cognitive disease are not the same thing.
Mental health
fromwww.scientificamerican.com
1 month agoAlzheimer's blood tests may predict when a person will develop symptoms
But questions remain about the accuracy and uncertainty of these tests, and experts caution that the assays aren't ready for prime time. While the results here are encouraging, they are not yet at the level of having significant clinical benefit for individual patients, says Corey Bolton, a clinical neuropsychologist and an assistant professor of medicine at Vanderbilt University Medical Center, who was not involved in the new study.
Medicine
Science
fromNews Center
2 months agoTargeting Key Proteins in Fight Against ALS - News Center
RAD23 controls both degradation and stabilization of misfolded proteins; reducing RAD23 enhances clearance of disease-linked aggregates, offering a therapeutic target for neurodegenerative proteostasis dysfunction.
fromSilicon Canals
1 month agoA brain-based AI test could point to the best antidepressant for you - Silicon Canals
Before treatment began, participants underwent neuroimaging. Instead of relying on a single modality, the researchers fused structural connectivity (how regions are physically wired) with functional connectivity (how regions co-activate at rest). The goal was not to throw every possible feature at a black box, but to learn a constrained pattern-what the authors call structure-function "covariation"-that carries the most predictive signal for outcome. In other words, the model tries to find the smallest set of connections that meaningfully forecasts symptom change.
Mental health
fromwww.nytimes.com
2 months agoBrain Health Challenge: Try a Brain Teaser
Decades of research show that people who have more years of education, more cognitively demanding jobs or more mentally stimulating hobbies all tend to have a reduced risk of cognitive impairment as they get older. Experts think this is partly thanks to cognitive reserve: Basically, the more brain power you've built up over the years, the more you can stand to lose before you experience impairment.
Public health
fromPsychology Today
2 months agoThe Inflamed Brain in Psychiatric Disorders
A recent study published in Biological Psychiatry identified a distinct subtype of psychiatric illness marked by brain inflammation, one that cuts across traditional diagnoses and may explain why standard treatments fail for some people (Tang et al., 2025).This new brain imaging study offers an interesting clue. It turns out that across different psychiatric disorders, some people show clear signs of brain inflammation, visible on scans and confirmed through immune system tests.
Mental health
fromNature
2 months agoUntangling the connection between dopamine and ADHD
Haavik was surprised to hear this because the scientific data do not suggest an unequivocal link between low levels of the neurotransmitter dopamine and ADHD. But the idea that low dopamine is a direct cause of ADHD is a common misconception, one that's amplified on social media and even in popular books about the condition. The reality, Haavik and other researchers say, is that the causes of ADHD are more diverse and nuanced than a simple deficit in one chemical cue in the brain.
Science
fromwww.theguardian.com
2 months agoAlzheimer's therapies should target a particular gene, researchers say
New therapies for Alzheimer's disease should target a particular gene linked to the condition, according to researchers who said most cases would never arise if its harmful effects were neutralised. The call to action follows the arrival of the first wave of drugs that aim to treat Alzheimer's patients by removing toxic proteins from the brain. While the drugs slow the disease down, the benefits are minor,
Medicine
Medicine
fromSilicon Canals
1 month agoIf you're over 65 and these 8 things come naturally to you, your cognitive health is exceptional - Silicon Canals
Certain habits and abilities—like learning new technology, strong memory for recent conversations, and cognitive flexibility—predict preserved memory and brain health in older adults.
fromMail Online
1 month agoBacteria found the eyes could drive dementia, experts discover
To make their discovery, researchers examined donated eye tissue from more than 100 people who had died with Alzheimer's, mild cognitive impairment or no signs of dementia. They were looking specifically for C. pneumoniae, because previous research has already linked it to Alzheimer's. The bacteria has also been detected in brain tissue from patients who died with the condition, sometimes found close to the sticky amyloid plaques and tangles believed to drive memory loss and confusion.
Medicine
fromNature
1 month agoDaily briefing: Caffeine might reduce dementia risk and slow cognitive decline
Researchers used data from two health studies to track the caffeine-drinking habits of more than 130,000 people over four decades. They found that drinking 2-3 cups of coffee or 1-2 cups of tea a day was associated with the greatest reductions in rate of cognitive decline, a result that held true even in people with a genetic variant called APOE4, which is associated with Alzheimer's disease.
Medicine
fromNature
2 months agoStill conscious? Brain marker signals when anaesthesia takes hold
They then used emerging mathematical methods to isolate signals originating from nine brain regions previously implicated in mediating consciousness and examined connections between pairs of these regions. Among them were the parietal cortex, which is at the top of the brain about halfway between the forehead and the back of the skull; the occipital cortex, at the back of the head; and several small, deeper structures, such as one called the thalamus.
Medicine
fromTNW | Deep-Tech
1 month agoAerska raises $39M to help RNA medicines reach the brain
For families living with neurodegenerative disease, the hardest part is not always the diagnosis. It is the slow erosion that follows: memory fading, personality shifting, independence shrinking. It unfolds quietly. First, forgotten appointments. Then repeated questions. Then moments when a familiar face no longer feels familiar. The illness does not isolate itself to one body. It rearranges the lives around it.
Medicine
fromNews Center
2 months agoPost-Stroke Injection Protects the Brain in Preclinical Study - News Center
When a person suffers a stroke, physicians must restore blood flow to the brain as quickly as possible to save their life. But, ironically, that life-saving rush of blood can also trigger a second wave of damage - killing brain cells, fueling inflammation and increasing the odds of long-term disability. Now, in a study published in the journal Neurotherapeutics, Northwestern University scientists have developed an injectable regenerative nanomaterial that helps protect the brain during this vulnerable window.
Medicine
fromBig Think
2 months agoWhy even the healthiest people hit a wall at age 70
If we really invest in longevity science, we have a chance to build a better future. It's gonna be better in one very simple way. There's gonna be a lot less disease. At the moment, aging is the leading cause of death globally. Over a hundred thousand people die every single day of cancer, of Alzheimer's, of the increased risk of infectious disease that comes along with growing older.
Medicine
[ Load more ]