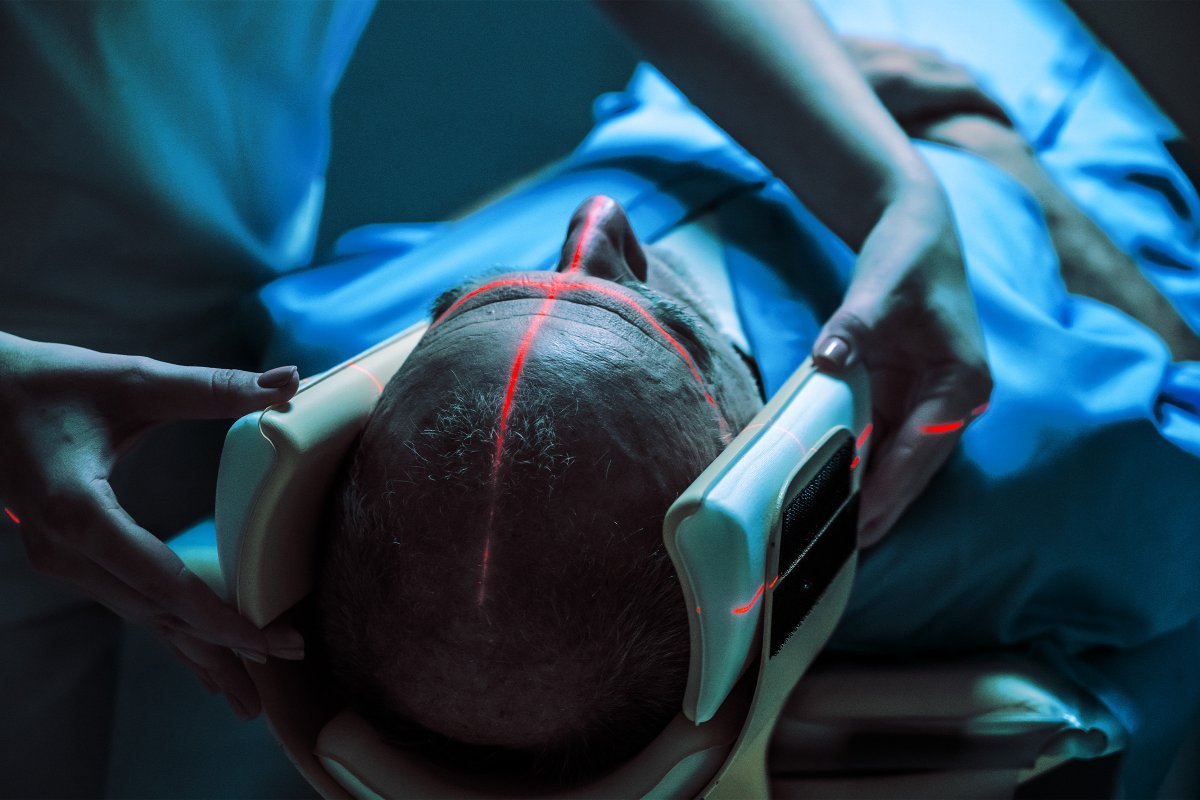
#robotics-and-medical-imaging
#robotics-and-medical-imaging
[ follow ]
#ai
Medicine
fromwww.businessinsider.com
1 hour agoI vibe coded an AI tool to help my mom fight stage 4 cancer. It helped us catch errors in her treatment and let her die with dignity.
Pratik Desai developed a tool to assist his mother in navigating Stage 4 duodenal adenocarcinoma using advanced coding and AI technology.
fromTNW | Startups-Technology
1 day agoWearable Robotics raises 5M to expand its arm exoskeleton
The ALEX RS is a bilateral upper-limb exoskeleton designed for post-stroke rehabilitation, covering 92% of the human arm's natural range of motion and is CE certified as a Class IIa medical device.
European startups
fromdesignboom | architecture & design magazine
5 days agobody agency and the ways wearable devices let people regain control of their physical forms
Body agency is a power returned after an incident took it away from the user's physical form, and some wearable devices and technologies have this exact goal in mind.
Wearables
Women in technology
fromFuturism
2 weeks agoThis Video of a Humanoid Robot Playing Perfect Tennis Is Extremely Impressive
Chinese company Galbot developed software enabling a Unitree G1 humanoid robot to play tennis with sustained rallies, millisecond reactions, and precise ball striking against human opponents.
Information security
fromSecurityWeek
2 weeks agoRobotic Surgery Giant Intuitive Discloses Cyberattack
Intuitive Surgical suffered a targeted phishing cyberattack resulting in unauthorized access to internal business applications and customer data, but robotic systems and manufacturing operations remained unaffected.
fromdesignboom | architecture & design magazine
2 weeks agostretchable robotic fingers for surgery decomposes in soil and becomes fertilizer
The body of the robotic fingers is built from polyglycerol sebacate, a synthetic elastomer made from glycerol and sebacic acid. Glycerol is a byproduct of biodiesel production while sebacic acid is derived from castor oil, and both of them are plant-based. Polyglycerol sebacate is safe since it is already used in medical implants because the body can absorb it without a toxic response.
Science
Russo-Ukrainian War
fromBusiness Insider
3 weeks agoThe US Army wants to see if it can get robots to rescue wounded troops like they're doing in Ukraine
The US Army is testing ground robots to evacuate wounded soldiers in high-intensity combat, reducing risk to medical personnel and troops during dangerous battlefield movements.
#healthcare-ai
Healthcare
fromwww.mercurynews.com
1 month agoAmazon bets on health care AI with tools for patients, doctors
Amazon Web Services launches Amazon Connect Health, an AI tool that automates medical documentation, billing codes, patient verification, and appointment scheduling to reduce healthcare administrative burden.
Healthcare
fromHarvard Business Review
3 weeks agoHealthcare Uses Specialized Language. It Needs Specialized AI, Too.
Healthcare professionals across specialties use inconsistent terminology and communication styles, creating significant translation barriers that impede care coordination and data interoperability.
fromianVisits
1 month agoFlying drones and robot dogs being used to move medial samples between NHS hospitals
In 2024, the NHS began testing whether flying drones could do a better job than couriers shuttling blood samples between labs in Guy's and St Thomas' hospitals. Instead of weaving through traffic, the drones simply lifted off, crossed central London, and landed minutes later. Delivery times dropped to barely a couple of minutes, reliability shot up thanks to a lack of roadworks in the sky, and the service turned out to be cheaper too. Since then, more than 6,000 samples have been transported by air.
Public health
Healthcare
fromBusiness Matters
1 month agoPulse Radiology Education: Built Around the Working Technologist
Pulse Radiology Education addresses barriers to professional advancement for working radiologic technologists by combining flexible online education with guaranteed clinical placement partnerships.
fromFuturism
1 month agoAI-Powered Surgery Tool Repeatedly Injuring Patients, Lawsuits Claim
Artificial intelligence has taken the medical device industry by storm - even adding a layer of complexity to the operating room that's resulting in patients being hurt, some health professionals claim. As Reuters reports, the TruDi Navigation System by device maker Acclarent was designed to treat chronic sinusitis, inflammation of the nasal sinuses, by inserting a tiny balloon to enlarge the sinus cavity openings.
Medicine
fromFast Company
2 months agoConnected data will rescue healthcare
AI plays an important role-but not by fixing fragmented data on its own. The work of organizing, connecting, and interpreting healthcare information still belongs to people and the systems they build. Where AI helps is after that foundation is in place: by bringing the right information forward at the right time, reducing the effort it takes to find what matters, and supporting better decisions in the moment of care.
Medicine
fromBusiness Matters
2 months agoThe Life Imaging Fla Story: Why Timing Matters in Modern Healthcare
After losing both of his parents to cancer, Tom set out to challenge a healthcare system that often waits for symptoms instead of identifying risk early. What began in Deerfield Beach, Florida, has grown into a multi-location preventative imaging company serving communities across the state. Life Imaging Fla focuses on preventative heart and full-body screenings. These services give people access to advanced imaging that is typically only approved once symptoms appear. The goal is straightforward: identify disease earlier, when people still have time, options, and control.
Medicine
fromForbes
2 months agoWhy AI Chatbots Are Essential For Modern Medical Practices
The world of medical practice management is changing faster than ever, driven by two simultaneous forces: escalating patient expectations and crushing administrative complexity. In my years working with healthcare organizations, I've seen these challenges evolve from nuisances into crises. Research by Bain & Company found that 65% of healthcare consumers want more convenient experiences, and 70% want more responsiveness from providers. They want instant answers to routine questions, immediate scheduling access and minimal friction.
Healthcare
fromPsychology Today
2 months agoMy Dad Got Sick-Doctors Dodged, AI Didn't
My dad was in the emergency room, short of breath, chest tight, upper back aching. He looked pale and confused. An ultrasound showed excess fluid between his lung and chest wall. "We'll drain it," a resident said, as if he were unclogging a sink. For the next five days, thick, red-tinged fluid filled a plastic container beside my dad's hospital bed. Doctors sent his cells for "staining," a way to identify cancer. But no one used that word.
Medicine
fromNature
2 months ago48 hours without lungs: artificial organ kept man alive until transplant
A 33-year-old man survived for 48 hours without his lungs, after a medical team replaced the organs with an external artificial-lung system that it developed to keep him alive until he could receive a double lung transplant. There have been cases in which people have had their lungs removed and been connected to an external device to maintain oxygen levels.
Medicine
[ Load more ]